Deciding whether an implant tooth procedure is right for you can feel overwhelming. This post will help you understand what an implant tooth procedure involves, who makes a good candidate, what to expect during treatment, the benefits and risks, cost and timeline factors, and how a coordinated team can improve outcomes. Use this guide to decide if you should bring your questions to a consultation.
What is an implant tooth procedure?
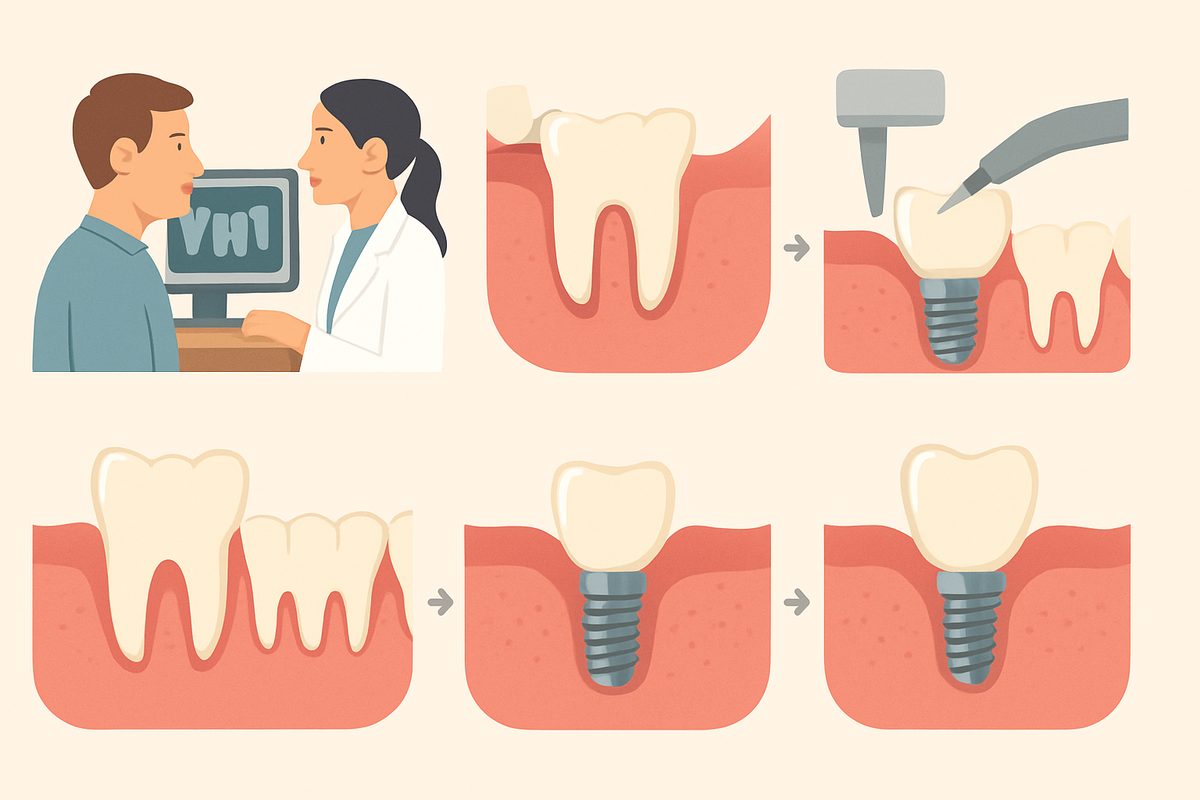
An implant tooth procedure replaces a missing tooth with three main parts: a titanium implant placed into the jawbone, an abutment that connects the implant to the visible tooth, and a crown that looks and works like a natural tooth. Unlike a bridge that relies on adjacent teeth or a removable denture, an implant is anchored in the bone and functions much like a natural root.
Because implants fuse with bone, they help preserve jawbone volume and often feel more stable for chewing and speaking than removable options.
Who is a good candidate for an implant tooth procedure?
Many adults with one or more missing teeth can be good candidates, but success depends on oral health, medical history, and lifestyle.
Oral health and bone needs
Implants need enough healthy bone to hold them steady. If bone volume is low, bone grafting can rebuild the area. Healthy gums free of active infection are also important because gum disease can threaten implant success. Your dentist will check bone with imaging and a clinical exam.
Medical conditions and medications
Certain conditions affect healing. Poorly controlled diabetes, autoimmune disorders, or cancer treatments can raise risk. Medications such as bisphosphonates or strong immunosuppressants may require special planning. Always share your full medical history and medications so your dental team can coordinate care with your physician if needed.
Lifestyle factors
Smoking lowers success rates and slows healing. Good oral hygiene and realistic expectations about maintenance are essential. Heavy clenching or grinding (bruxism) should be managed with a nightguard or other treatment to protect the implant over time.
What to expect during an implant tooth procedure
Planning and imaging
Careful planning starts with digital scans and a CBCT 3D image to map bone and nearby anatomy. Computer-guided planning helps place the implant in the best position for function and esthetics, reducing surprises during surgery.
Surgery and sedation options
On surgery day the implant is placed through a small incision in the gum and secured into the jaw. Sedation options include nitrous oxide, oral sedation, or IV sedation depending on the case and patient comfort. After surgery you will receive instructions for pain control, antibiotics if needed, and soft-food care.
Healing and final restoration
Bone integrates with the implant over several weeks to months. A temporary crown or prosthesis may be used while healing occurs. Once integration is confirmed, the final crown is attached. Practices with an in-house lab can shorten the timeline for custom crowns and let clinicians verify shade and fit faster.
Benefits, risks, and alternatives
- Benefits: stable chewing, bone preservation, long-term durability, improved appearance and confidence.
- Risks: infection, implant failure, nerve or sinus complications (rare), need for additional grafting.
Alternatives include a fixed bridge or a removable partial denture. A bridge may be preferred when nearby teeth are healthy and you want a shorter timeline. A partial denture can be a lower-cost, non-surgical option. Your dentist can explain which choice suits your oral health and goals.
Cost, timeline, and financing considerations
Cost depends on factors like single-tooth vs. multiple implants, need for grafting or sinus lifts, and choice of materials (titanium vs. zirconia). Timelines range from a few months for a straightforward single tooth to longer when grafting or staged treatments are needed. Many practices offer payment plans, third-party financing (like CareCredit), and help navigating insurance benefits to make treatment more affordable.
Why choose a multidisciplinary team for complex implant tooth procedures?
For complex cases, coordinated care from a prosthodontist and an oral surgeon improves predictability. A team can plan surgery and the final restoration together, using on-site CBCT, digital scans, guided surgery, and an in-house lab for faster, precise results. At Dental Associates of Colorado, for example, prosthodontist Seung H. Lee, DDS and oral & maxillofacial surgeon Jonathan Jundt, MD, DDS lead a team that offers sedation options, on-site 3D imaging, and an experienced in-house crown and denture lab to speed care and reduce remakes.
Next steps: Is an implant tooth procedure right for you?
Bring this quick checklist to your consultation:
- List of medical conditions and current medications
- Any dental X-rays or bitewing images you have
- Your goals for function and appearance
- Questions about timeline, costs, and sedation
At the initial exam expect a review of your health, a clinical exam, and digital imaging. If you’re ready to learn more, schedule a consultation to get a personalized plan and clear next steps for whether an implant tooth procedure is right for you.